
Start improving efficiency, reducing workload, and achieving better outcomes today.

Provider credentialing is the process of verifying and enrolling healthcare providers with insurance networks. It ensures that providers meet all requirements to offer services and receive reimbursements from payers.
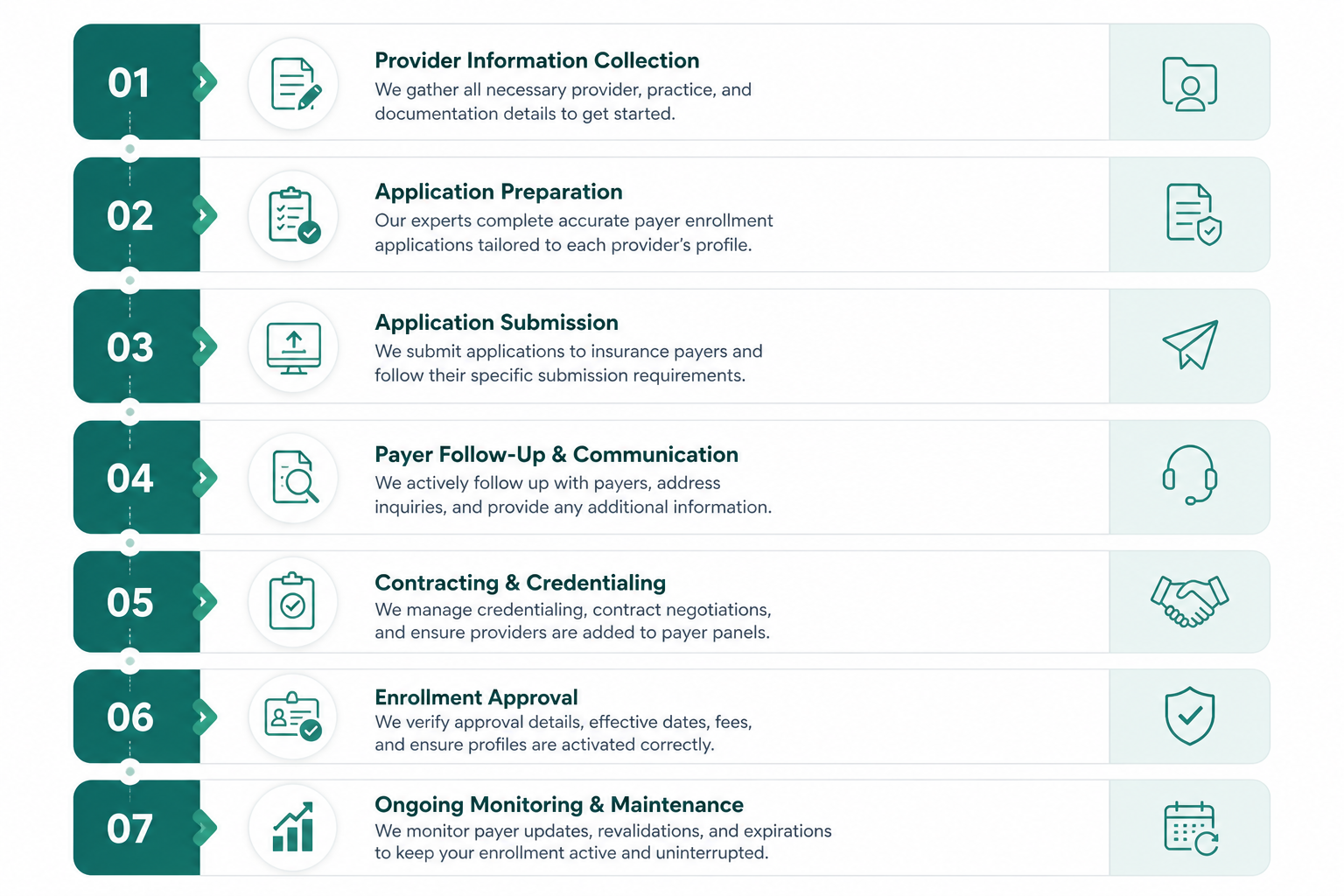
At Carenex RCM, we streamline credentialing to avoid delays, reduce errors, and ensure smooth participation with insurance companies.
Complete provider enrollment with commercial and government payers.
Timely renewals to maintain uninterrupted participation.
Accurate setup and maintenance of CAQH profiles.
Regular follow-ups to speed up approvals and avoid delays.
Review existing profiles to identify errors and gaps.
Maintain accurate and updated provider information.

With a structured credentialing process, Carenex RCM helps you eliminate delays, maintain compliance, and ensure smooth participation with insurance networks.
99% First-Time Approval Rate
Most delays come from small mistakes. Our medical billing and credentialing experts check every detail so your applications are payer-ready and move forward.
Dedicated Enrollment Manager
Work with one dedicated credentialing specialist who knows your timelines, payers, and practice, no tickets, no confusion—just a superior credentialing experience.
Payer Enrollment in all 50 States
From one plan to nationwide growth, we manage commercial payer enrollment and Medicare credentialing services, Medicaid and specialty payers across 50 states.
Weekly Status Updates
We track every application and share biweekly updates so your payer enrollment keeps moving forward—no guessing, only clear progress to approval.
Better Payer Contracts
We correct outdated data sync documents and maintain your CAQH profile, ensuring that every payer request moves faster without delays, stalled files, or missed updates.
Reduced Claim Denials
We review claims carefully to minimize denials and rejections.
Cost Efficiency
Reduce overhead costs by outsourcing billing and administrative tasks.
HIPAA Compliance
Strict compliance ensures complete data security and patient confidentiality.

Faster Payments
Optimized billing ensures quicker reimbursements and improved cash flow.
Consistent AR Follow-Up
Regular follow-ups ensure maximum collections and fewer outstanding balances.
Accurate Medical Coding
Certified coders ensure accurate coding and error-free claim submissions.










Get Credentialed Without Delays
Ensure smooth provider enrollment and faster approvals with expert credentialing support.
Get Solutions From Our Specialists
Carenex RCM has been helping me obtain my credentials with various medical insurance providers. He is knowledgeable and responsive, which made the entire process smooth and easy.
I can't recommend Carenex enough for their outstanding credentialing services (speech therapy). From start to finish, their team was incredibly professional, knowledgeable, and responsive. If you're looking for a smooth, efficient credentialing experience with people who genuinely care about your success, this is the team you want on your side!